This month's Kidney International has a special extra edition on Chronic renal allograft dysfunction.
This supplement has >10 articles that highlights latest development in transplantation on pathogenetic mechanisms of T and B cells in Chronic rejection, IF/TA and then few chapters on fibrosis and genomic studies.
Risk factors, infections and immune monitoring are also discussed.
Few of them are linked below:
http://www.ncbi.nlm.nih.gov/pubmed
http://www.ncbi.nlm.nih.gov/pubmed/21116312
http://www.ncbi.nlm.nih.gov/pubmed/21116316
Saturday, December 25, 2010
Tuesday, December 21, 2010
CMV in solid Organ transplantation!
CMV infections are fairly common in solid organ transplantations. A nice review in Nature Review Nephrology this month highlights prophylaxis treatment, active treatment and serology testing. What I found very useful wa a table on dosage recommendations for ganciclovir and valganciclovir in varied renal function states.
A nice section on anti viral resistance also reveals some important data on use of foscarnet and when there is UL97 mutations. These strains usually have ganciclovir resistance. The UL54 strain mutation can have resistance to even foscarnet and cidofivir. The advent of commercially available genotyping allows for rapid results of UL97 or 54 and allow for personalized treatment of CMV viremia or disease.
Resistant CMV guidelines
1. Increase dose of ganciclovir
2. Change to foscarnet with or without continued ganciclovir
3. Change to Cidofovir only if pol mutations are not present otherwise it cross reacts with ganciclovir resistance.
4. leflunomide has been tried in few cases.
5. CMV immunoglobulin (IVIG) as a last resort and if there is organ damage happening.
Check it out
Saturday, December 18, 2010
Genetic Nephropathies and Kidney Transplantation
A recent article in Nature Review Nephrology reviews the diseases we always get worried if a living donor can be used.
This review outlines the does and don't of hereditary nephropathies and donor evaluation of kidney transplantation. A table in the articles nicely summarizes the disease entity and if the living related donation would be appropriate.
In Finnish type Congenital Nephrotic syndrome, NPHS2 FSGS, NPHS3 FSGS, Pierson Syndrome, Schimke's immunoosseous dystrophy, nephronophthisis, cystinosis and ARPKD and alport syndrome:- it is ok to use living related donation in transplantation. In Primary Hyperoxaluria and Atypical HUS, one has to be careful in selecting the donor from a living relative.
In general AR type of diseases, the donor can be a relative and most of the time its not a problem. Autosomal Dominant diseases is always a concern. We come across this most in ADPKD and the donor evaluation in that case is so strict and needs careful screening if its a relative. Atypical HUS should not receive a kidney transplantation from a living donor because it is a high risk for disease recurrence and graft loss.
Ref:
http://www.ncbi.nlm.nih.gov/pubmed/20877305
This review outlines the does and don't of hereditary nephropathies and donor evaluation of kidney transplantation. A table in the articles nicely summarizes the disease entity and if the living related donation would be appropriate.
In Finnish type Congenital Nephrotic syndrome, NPHS2 FSGS, NPHS3 FSGS, Pierson Syndrome, Schimke's immunoosseous dystrophy, nephronophthisis, cystinosis and ARPKD and alport syndrome:- it is ok to use living related donation in transplantation. In Primary Hyperoxaluria and Atypical HUS, one has to be careful in selecting the donor from a living relative.
In general AR type of diseases, the donor can be a relative and most of the time its not a problem. Autosomal Dominant diseases is always a concern. We come across this most in ADPKD and the donor evaluation in that case is so strict and needs careful screening if its a relative. Atypical HUS should not receive a kidney transplantation from a living donor because it is a high risk for disease recurrence and graft loss.
Ref:
http://www.ncbi.nlm.nih.gov/pubmed/20877305
Friday, December 10, 2010
Quiz 9 Answers
Which drug is paired incorrectly with the target molecule?
Rituximab -- CD20
Alemtuzumab -- CD52
Belatacept -- CD198
Belimumab --- TNFSF13B
Atacicept ---TACI-Ig
The correct answer is Belatacept CD198, that is incorrect pairing. Most of you got it right.
We all are familiar with Rituximab which is a B cell antagonist and since all B cells besides plasma cells are CD20 Positive, its an anti CD20. Alemtuzumab(campath) targets cd52 a protein present on the surface of mature lymphocytes. Atacicept(TACI-Ig) is a human recombinant fusion protein that comprises the binding portion of a receptor for both BLyS (B-Lymphocyte Stimulator) and APRIL (A PRoliferation-Inducing Ligand), two cytokines that have been identified as important regulators of B-cell maturation, function and survival. Atacicept has shown selective effects on cells of the B-cell lineage, acting on mature B cells and blocking plasma cells and late stages of B-cell development while sparing B-cell progenitors and memory cells. The efficacy of atacicept in animal models of autoimmune disease and the biological activity of atacicept in patients with systemic lupus erythematosus (SLE) and rheumatoid arthritis (RA) has been demonstrated. The selective inhibitor of T-cell costimulation, belatacept, blocks CD28-mediated T-cell activation by binding CD80 and CD86 on antigen-presenting cells. Understanding the extent to which belatacept binds to its targets in patients may enable correlation of belatacept exposure to receptor saturation as a pharmacodynamic measure of costimulation blockade. Belimumab (registered name Benlysta previously known as LymphoStat-B), is a fully human monoclonal antibody that specifically recognizes and inhibits the biological activity of B-Lymphocyte stimulator (BLyS), also known as B cell activation factor of the TNF family (BAFF).
Labels:
Immunology,
Immunosuppresion,
quiz
Friday, December 3, 2010
Sirolimus- the Positive aspects
The same issue of KI shares another view- the positive aspects of sirolimus
As we mentioned earlier that this agent was discovered as a cancer drug and has antiproliferative properties
Recent animal data and human data have shown it to be beneficial in preventing cancer post transplant
So the benefits of this agents are:
1. Prevention of cancer, as mTOR is responsible for transcription and translation for cell growth. Definite evidence against Kaposi, Skin cancers and renal cancers.
2. Increase in T regs
3. Anti viral effects - CMV, BK and EBV viral infections ( still not sure- conflicting data)
4. Tolerance inducing potential
5. Control of fibrotic process - conflicting data when compared to CNI alone
Ref:
http://www.ncbi.nlm.nih.gov/pubmed/20981120
As we mentioned earlier that this agent was discovered as a cancer drug and has antiproliferative properties
Recent animal data and human data have shown it to be beneficial in preventing cancer post transplant
So the benefits of this agents are:
1. Prevention of cancer, as mTOR is responsible for transcription and translation for cell growth. Definite evidence against Kaposi, Skin cancers and renal cancers.
2. Increase in T regs
3. Anti viral effects - CMV, BK and EBV viral infections ( still not sure- conflicting data)
4. Tolerance inducing potential
5. Control of fibrotic process - conflicting data when compared to CNI alone
Ref:
http://www.ncbi.nlm.nih.gov/pubmed/20981120
Tuesday, November 30, 2010
Sirolimus - The negative aspects
A recent article in Kidney International discusses the negative and positive aspects of this interesting drug- sirolimus, mTOr inhibitor. Initially designed to fight renal cancer, fast caught on to treat rejection and be used as an immunosuppression.
1. Six trials so far have randomized sirolimus vs a calcineurin inhibitor that were mentioned in this article. They all had more acute rejection episodes with sirolimus. So graft survival is a concern.
2. Renal toxicity has been described- from TMA to collapsing FSGS and severe proteinuria making it not as promising as CNI. But CNI have a more chronic toxicity to the kidney
3. Dyslipidemia has been noted as well more with this agent. - close to 60% of the patients getting mTor in clinical trials required lipid lowering agents
4. NODAT was also noted to be higher in this group; 25% more chance than CNI
5. Wound healing:- preventing the surgical wound healing or in future if patients need other surgeries makes it tough.
6. Other- mouth ulcers, myelosuppresion and infertility were more common in this agent as well.
7. Finally, they mention the new findings lately described pulmonary toxicities that are leading to a restrictive disease in the lung.
Ref:
http://www.ncbi.nlm.nih.gov/pubmed/20703217
1. Six trials so far have randomized sirolimus vs a calcineurin inhibitor that were mentioned in this article. They all had more acute rejection episodes with sirolimus. So graft survival is a concern.
2. Renal toxicity has been described- from TMA to collapsing FSGS and severe proteinuria making it not as promising as CNI. But CNI have a more chronic toxicity to the kidney
3. Dyslipidemia has been noted as well more with this agent. - close to 60% of the patients getting mTor in clinical trials required lipid lowering agents
4. NODAT was also noted to be higher in this group; 25% more chance than CNI
5. Wound healing:- preventing the surgical wound healing or in future if patients need other surgeries makes it tough.
6. Other- mouth ulcers, myelosuppresion and infertility were more common in this agent as well.
7. Finally, they mention the new findings lately described pulmonary toxicities that are leading to a restrictive disease in the lung.
Ref:
http://www.ncbi.nlm.nih.gov/pubmed/20703217
Thursday, November 18, 2010
The Kidney Transplant in HIV patients- the NEJM study
Kidney Transplantation was rare in HIV+ cases few years ago and now many centers have developed protocols that have allowed this to happen with relatively good outcomes.
No prospective studies were ever done in this matter for rejection rates, outcome measures and so forth,
This month in NEJM 2010, a nice multi center study takes a look at this particular question. The investigators evaluated 150 patients for close to 2 years, multicenter fashion, non randomized prospective fashion.
The mean graft survival was 90% at one year and 3 years was 73.7%. The ones that didn't do well were the ones with rejection episodes, use of thymoglobulin, and non living donors. The rejection rate was higher than expected, close to 31% at 1 year and 41% in 3 years.
This study shows that graft survival is good but the rejection rates are high still and needs some work. Perhaps the drug interaction with HAART therapy play a role in the fluctuation of perhaps CNI levels and higher rejection risk or the immunosuppresive agents we have now are not the ideal ones for an immunodeficiency diseases model?
ref:
http://www.nejm.org/doi/full/10.1056/NEJMoa1001197
http://www.ncbi.nlm.nih.gov/pubmed/19776780
No prospective studies were ever done in this matter for rejection rates, outcome measures and so forth,
This month in NEJM 2010, a nice multi center study takes a look at this particular question. The investigators evaluated 150 patients for close to 2 years, multicenter fashion, non randomized prospective fashion.
The mean graft survival was 90% at one year and 3 years was 73.7%. The ones that didn't do well were the ones with rejection episodes, use of thymoglobulin, and non living donors. The rejection rate was higher than expected, close to 31% at 1 year and 41% in 3 years.
This study shows that graft survival is good but the rejection rates are high still and needs some work. Perhaps the drug interaction with HAART therapy play a role in the fluctuation of perhaps CNI levels and higher rejection risk or the immunosuppresive agents we have now are not the ideal ones for an immunodeficiency diseases model?
ref:
http://www.nejm.org/doi/full/10.1056/NEJMoa1001197
http://www.ncbi.nlm.nih.gov/pubmed/19776780
Labels:
clinical science,
Infections,
kidney transplantation
Wednesday, November 3, 2010
Quiz 8 answers
Immunology Quiz: There are two types of Tregs:- the natural kind and the induced kind. Which of these statements is FALSE?
1.The natural T regs are thymus derived 0 (0%)
2.The induced T regs are generated in the periphery 0 (0%)
3.The natural T regs are derived from T effector cells 5 (50%)
4.The natural T regs suppress autoimmunity 2 (20%)
5. The induced T regs induction requires CD28 signalling, and possibly TGF-B and other cytokines
1 (10%)
6.The natural T regs are selected by autoantigens
2 (20%)
There are two types of T regulatory cells, one that is natural Tregs and the other that is induced T regs.
But are Foxpe+T reg cells.
Natural T regs: are Thymus derived, selected by autoantigens and could be autoreactive.
They cross react to alloantigens and suppress autoimmunity.
Induced T regs: are generated in the periphery, derived from T effector cells. Their induction requires cytokine activation and CD28 signialling. They are positively and negatively regulated by many pathways.
Hence, the choice number 3 is wrong.
Nice review below:
Labels:
Immunology,
kidney transplantation,
quiz
Monday, November 1, 2010
Tuesday, October 26, 2010
Outcomes of kidney transplantation from HCV positive donors
 Given the global organ shortage for transplantation, use of expanded criteria donors and donors with potentially transmissible diseases has been established as a way to mitigate this problem somewhat. While there is universal consensus on rejecting kidneys from HCV antibody positive donors for transplantation in HCV antibody negative recipients, there is controversy regarding the use of these kidneys for HCV antibody positive recipients. Well, we have the first study that reported the long-term experience in this area (Morales et al, Am J Transplant. Nov 2010). This study was done in Spain. Outcomes of 162 HCV antibody positive recipients (97% of them are HCV RNA positive as well) that received a kidney from HCV antibody positive donors were compared with outcomes of 306 HCV antibody positive recipients that recieved kidney from HCV antibody negative donors. Mean follow-up was 74.5 months. There was no difference in patient survial and decompensated liver disease between the two groups. 5-year and 10-year graft survival was 58.9% and 34.4% versus 65.5% and 47.6% respectively (p = 0.006) while death-censored graft survival was 69% and 47% versus 72.7% and 58.5% (p = 0.055). Cox-regression analysis could not identify the donor's HCV serology as a significant risk factor for death, graft failure and severe liver disease in HCV antibody positive recipients. These findings prove that use of this strategy is safe and helps the problem of severe organ shortage that we are facing now.
Given the global organ shortage for transplantation, use of expanded criteria donors and donors with potentially transmissible diseases has been established as a way to mitigate this problem somewhat. While there is universal consensus on rejecting kidneys from HCV antibody positive donors for transplantation in HCV antibody negative recipients, there is controversy regarding the use of these kidneys for HCV antibody positive recipients. Well, we have the first study that reported the long-term experience in this area (Morales et al, Am J Transplant. Nov 2010). This study was done in Spain. Outcomes of 162 HCV antibody positive recipients (97% of them are HCV RNA positive as well) that received a kidney from HCV antibody positive donors were compared with outcomes of 306 HCV antibody positive recipients that recieved kidney from HCV antibody negative donors. Mean follow-up was 74.5 months. There was no difference in patient survial and decompensated liver disease between the two groups. 5-year and 10-year graft survival was 58.9% and 34.4% versus 65.5% and 47.6% respectively (p = 0.006) while death-censored graft survival was 69% and 47% versus 72.7% and 58.5% (p = 0.055). Cox-regression analysis could not identify the donor's HCV serology as a significant risk factor for death, graft failure and severe liver disease in HCV antibody positive recipients. These findings prove that use of this strategy is safe and helps the problem of severe organ shortage that we are facing now.
Salivary Prograf levels
Check out this interesting post from Pediatric Nephrology on salivary tacrolimus levels
https://www.pediatric-nephrology.com/daily-updates/2010/10/26/329-salivatac.html
https://www.pediatric-nephrology.com/daily-updates/2010/10/26/329-salivatac.html
Labels:
Immunosuppresion,
kidney transplantation
U 002 Nierentransplantation / kidney transplant
A nice you tube video ( cartoon) of a transplant surgery
Sunday, October 24, 2010
FGF-23 and PTH and Bone Disease post transplant
Patients with ESRD have bone disease of various types. The three that are commonly seen are adynamic bone disease, increased bone turnover related or a combination of both.
BMD loss is common complication following kidney transplantation.
Few points to take home from a recent paper published in CJASN 2010, October edition.
1. The bone loss is accelerated in the post transplant period- why? Steroids and perhaps CNI worsen the rate.
2. Other risk factors are pre existing renal disease, hypogonadism, and metabolic acidosis.
3. 90% of post transplant patients have hypophosphatemia( CNI related and or tertiary hyperparathyroidism)
4. Renal phosphate wasting has bad effects on bone
5. The renal phosphate wasting in part might be caused by elevated FGF23 levels or phosphatonin hormone.
6. PTH levels don't return completely to normal in most transplant patients post transplant
7. FGF 23 levels usually return to normal after one year post transplant
8. A recent study found that a high FGF23 level and low pth at time of transplant are the highest risk of developing bone disease post transplant
9. The most common bone biopsy finding post transplant is adynamic bone disease.
Image source: clipartheaven.com
References:
http://www.ncbi.nlm.nih.gov/pubmed/20634326
http://www.ncbi.nlm.nih.gov/pubmed/17359508
http://www.ncbi.nlm.nih.gov/pubmed/16941023
BMD loss is common complication following kidney transplantation.
Few points to take home from a recent paper published in CJASN 2010, October edition.
1. The bone loss is accelerated in the post transplant period- why? Steroids and perhaps CNI worsen the rate.
2. Other risk factors are pre existing renal disease, hypogonadism, and metabolic acidosis.
3. 90% of post transplant patients have hypophosphatemia( CNI related and or tertiary hyperparathyroidism)
4. Renal phosphate wasting has bad effects on bone
5. The renal phosphate wasting in part might be caused by elevated FGF23 levels or phosphatonin hormone.
6. PTH levels don't return completely to normal in most transplant patients post transplant
7. FGF 23 levels usually return to normal after one year post transplant
8. A recent study found that a high FGF23 level and low pth at time of transplant are the highest risk of developing bone disease post transplant
9. The most common bone biopsy finding post transplant is adynamic bone disease.
Image source: clipartheaven.com
References:
http://www.ncbi.nlm.nih.gov/pubmed/20634326
http://www.ncbi.nlm.nih.gov/pubmed/17359508
http://www.ncbi.nlm.nih.gov/pubmed/16941023
Saturday, October 23, 2010
Aspergilloma in the transplant kidney
A recent issue of AJKD talks about a case of aspergilloma in the transplanted kidney. The fact that it affected the kidney is the novelty of the case and the also they used a novel way of treating this patient. Please see the link below.
http://www.ajkd.org/article/S0272-6386(10)01257-6/fulltext
http://www.ajkd.org/article/S0272-6386(10)01257-6/fulltext
Thursday, October 21, 2010
Renal Fellow Network: Pancreas transplant pearls
Renal Fellow Network: Pancreas transplant pearls: "Pancreas transplantation is considered the treatment of choice for patients with refractory Type I Diabetes Mellitus. The first pancreas tr..."
Tuesday, October 19, 2010
Wait list and desensitization?
Two landmark papers have discussed using potential agents for potential patients who are on wait list for a kidney but have a very high PRA or now one might use a cPRA.
So the only data we have on what to use in highly sensitized DSA+ patients on the WAITING list is IVIG and rituximab perhaps? ( smaller study).
References:
http://www.ncbi.nlm.nih.gov/pubmed/15579530
http://www.ncbi.nlm.nih.gov/pubmed/18635429
Labels:
clinical science,
kidney transplantation
Sunday, October 17, 2010
Sirolimus and Male Fertility
 I just came across an interesting paper published couple of years ago. Zuber et al (Am J Transplantion,July 2008) carried out an observational study in male patients aged 20-40 years who received a kidney transplant during 1995-2005 in France. Patients on sirolimus based immunosuppression had a significantly reduced total sperm count and a decreased proportion of motile spermatozoa compared to patients who did not receive sirolimus. Also, it was found that the fathered pregnancy rate (pregnancies/1000 patient years) was 5.9 and 92.9 in patients receiving sirolimus-based and sirolimus-free regimens, respectively. Of those patients in whom sirolimus treatment was interrupted, only half of the patients showed a significant improvement in sperm parameters. The authors concluded that sirolimus is associated with impaired spermatogenesis and may reduce male fertility. So, if you have a male transplant patient on sirolimus presenting with fertility issues, switching sirolimus to another agent like tacrolimus may help.
I just came across an interesting paper published couple of years ago. Zuber et al (Am J Transplantion,July 2008) carried out an observational study in male patients aged 20-40 years who received a kidney transplant during 1995-2005 in France. Patients on sirolimus based immunosuppression had a significantly reduced total sperm count and a decreased proportion of motile spermatozoa compared to patients who did not receive sirolimus. Also, it was found that the fathered pregnancy rate (pregnancies/1000 patient years) was 5.9 and 92.9 in patients receiving sirolimus-based and sirolimus-free regimens, respectively. Of those patients in whom sirolimus treatment was interrupted, only half of the patients showed a significant improvement in sperm parameters. The authors concluded that sirolimus is associated with impaired spermatogenesis and may reduce male fertility. So, if you have a male transplant patient on sirolimus presenting with fertility issues, switching sirolimus to another agent like tacrolimus may help.
Thursday, October 14, 2010
Quiz 7 Answers
What is the most common glomerular disease following Liver Transplantation?
Ig A Nephropathy | 7 (46%) |
Minimal Change Disease | 0 (0%) |
Membranous GN | 4 (26%) |
MPGN Type 1 | 4 (26%) |
When 105 renal biopsies were studied in patients with non renal transplants for causes of glomerular disease, the most common transplant where glomerular disease was seen was liver transplantation. If you exclude, Thrombotic microangiopathy over glomerular disease, the most common was IgA Nephropathy followed by MPGN type 1 ( likely secondary to Hepatitis C).
In Bone marrow transplantation:- the most common finding was Thrombotic Microangiopathy( likely drug related or bone marrow transplant nephropathy or radiation related) followed by minimal change disease and membranous GN( which is usually seen with GvHD)
In Heart transplantation, IgA topped the list again.
A nice review can be found below:
Tuesday, October 12, 2010
New Transplant Information website
Check out this excellent website on information on transplantation
http://www.kidneylink.org/
It has medical news, patient stories, webinars and useful links to all transplant readership
http://www.kidneylink.org/
It has medical news, patient stories, webinars and useful links to all transplant readership
Labels:
Education,
kidney transplantation
Friday, October 8, 2010
REJECTION and TOLERANCE
This week is a transplant week in the journals.
The NEJM has a nice review on Rejection of the Kidney Allograft. Have a look. its very well written and combines the latest information on all concepts of rejection(with excellent visual portrayals)
Antibody Mediated and Cellular Mediated are discussed. It even goes into details of T cell activation and co stimulation and is a simple read for all.
It ends with a nice summary on even Late Acute rejection and Chronic Rejection
Another treat this week is the Nephrology Nature Review Journal- features an entire issue on Transplantation Tolerance, the holy grail of Transplantation. It reviews nice articles on Tolerance review, T Regs, Tregs and B cell interactions, Mixed chimerism and Biomarkers and proteonomics in transplant tolerance.
The references are below:
http://www.nejm.org/doi/full/10.1056/NEJMra0902927
http://www.ncbi.nlm.nih.gov/pubmed/20717099
The NEJM has a nice review on Rejection of the Kidney Allograft. Have a look. its very well written and combines the latest information on all concepts of rejection(with excellent visual portrayals)
Antibody Mediated and Cellular Mediated are discussed. It even goes into details of T cell activation and co stimulation and is a simple read for all.
It ends with a nice summary on even Late Acute rejection and Chronic Rejection
Another treat this week is the Nephrology Nature Review Journal- features an entire issue on Transplantation Tolerance, the holy grail of Transplantation. It reviews nice articles on Tolerance review, T Regs, Tregs and B cell interactions, Mixed chimerism and Biomarkers and proteonomics in transplant tolerance.
The references are below:
http://www.nejm.org/doi/full/10.1056/NEJMra0902927
http://www.ncbi.nlm.nih.gov/pubmed/20717099
Labels:
Immunology,
kidney transplantation,
rejection
Tuesday, October 5, 2010
Basic concepts in Immunology
Concept 1
Think of Innate immune system as "non antigen presenting mediated". it can get activated without antigen presentation. Cells that are major players: NK cell and Macrophage
Adaptive immune system is " antigen presentation mediated". Needs that extra help.
Cells that play role here:- B cells, T cells, DC
Concept 2
Think of the immune system as : Effector system and Regulatory system
Effector systems play a role in causing inflammation and damage and " doing their job" best!!! CD4+T, CD8+T cells, NK cells, B effector cells are all major players
Regulators are the "policemen". They are the Tregs and Bregs. They are out there trying to shut out fires and inflammation and try to "tone down" the reaction. Having more police around makes for a more robust and more "Controlled" immune system
Concept 3
The adaptive immune response has two arms
Afferent arm:-Antigen presentation
Efferent arm:- T cell activation
Concept 4
Two types of destruction:- cell mediated via Cd4 and Cd8 cells- granzyme and perforin and killing the cell
or antibody mediated via B cell-- leading to complement activation killing
Think of Innate immune system as "non antigen presenting mediated". it can get activated without antigen presentation. Cells that are major players: NK cell and Macrophage
Adaptive immune system is " antigen presentation mediated". Needs that extra help.
Cells that play role here:- B cells, T cells, DC
Concept 2
Think of the immune system as : Effector system and Regulatory system
Effector systems play a role in causing inflammation and damage and " doing their job" best!!! CD4+T, CD8+T cells, NK cells, B effector cells are all major players
Regulators are the "policemen". They are the Tregs and Bregs. They are out there trying to shut out fires and inflammation and try to "tone down" the reaction. Having more police around makes for a more robust and more "Controlled" immune system
Concept 3
The adaptive immune response has two arms
Afferent arm:-Antigen presentation
Efferent arm:- T cell activation
Concept 4
Two types of destruction:- cell mediated via Cd4 and Cd8 cells- granzyme and perforin and killing the cell
or antibody mediated via B cell-- leading to complement activation killing
Role Playing exercise in Transplant Education
We did another session of role playing with the fellows and transplant medicine
Each fellow was assigned a "cell" that is an active playing in Immunology. Then they were asked to describe themselves in Homeostasis and then a state of Immunosuppression. A nice discussion and arguments ensued and a live display of the immune reaction was done. The teaching of basic immunology for transplantation was mediated via this teaching method.
The cells the fellows' role played were: NK cell, macrophage, CD4+ T cell, CD8+T cell, DC, B effector cell, T Reg cell, B reg Cell.
Each fellow was assigned a "cell" that is an active playing in Immunology. Then they were asked to describe themselves in Homeostasis and then a state of Immunosuppression. A nice discussion and arguments ensued and a live display of the immune reaction was done. The teaching of basic immunology for transplantation was mediated via this teaching method.
The cells the fellows' role played were: NK cell, macrophage, CD4+ T cell, CD8+T cell, DC, B effector cell, T Reg cell, B reg Cell.
Labels:
clinical science,
Education,
Immunology
Wednesday, September 29, 2010
Transplant Glomerulopathy
Transplant Glomerulopathy(TG) is a common biopsy finding that we see in kidney biopsies for proteinuria workup.The causes of TG are usually of similar to what causes secondary MPGN. Most of the time it turns out to be chronic antibody mediated rejection process. Pathologically, it is defined by glomerular basement membrane duplication with peritubular capillary basement membrane multilayering (PTCML), and associated with anti-human leukocyte antigen antibodies and C4d.
A recent study in Transplantation 2010 issue talks about possible predictors of long term outcomes of pure TG cases. 36 cases were noted. Only 33% were c4D positive. but the C4d-positive cases also showed a trend toward rapid graft loss. Interstitial fibrosis, PTCML, and arteriolar hyalinosis were significant predictors of graft survival in TG. C4d positivity was associated with a more rapid rate of function decline. eGFR slope data showed significant deterioration in graft function well before the diagnostic biopsy.
References:
http://www.ncbi.nlm.nih.gov/pubmed/20838279
http://www.ncbi.nlm.nih.gov/pubmed/19594595
A recent study in Transplantation 2010 issue talks about possible predictors of long term outcomes of pure TG cases. 36 cases were noted. Only 33% were c4D positive. but the C4d-positive cases also showed a trend toward rapid graft loss. Interstitial fibrosis, PTCML, and arteriolar hyalinosis were significant predictors of graft survival in TG. C4d positivity was associated with a more rapid rate of function decline. eGFR slope data showed significant deterioration in graft function well before the diagnostic biopsy.
References:
http://www.ncbi.nlm.nih.gov/pubmed/20838279
http://www.ncbi.nlm.nih.gov/pubmed/19594595
Thursday, September 23, 2010
CMV and EBV PCR for 2 years
Check out this interesting post from Dr.Sethi
https://www.pediatric-nephrology.com/home/2010/09/23/300-jasnviremia.html
https://www.pediatric-nephrology.com/home/2010/09/23/300-jasnviremia.html
Labels:
Infections,
post transplant complications
B cells in Transplantation
Recently at the ATC 2010, a nice abstract was presented regarding Regulatory B cells. They are coming!!!
T cell immunglobulin and mucin -1 or TIM-1 is a costim molecule that controles T effector cells.
The listed abstract below showed that Tim-1 is more highly expressed on naive B cells than on T cells.
Depleting B cells led to Tim-1 accelerated islet cell rejection in these mice. Re constitution of B cells led to prolonged graft survival and and transfer of Tim-1 + B cells prolonged allograft survivial suggesting that Tim-1 + b cells could be B regulatory cells like Foxp3+ T reg cells.
Again, no human data yet. more studies to come!
Exciting stuff!
Reference:
Ding Q, Yueng M, Najafian N, et al. Regulatory B cells are identified by TIM-1 and can be induced through TIM-1 ligation to promote allograft survival. ATC 2010, San Diego, Calif, Abstract 167.
T cell immunglobulin and mucin -1 or TIM-1 is a costim molecule that controles T effector cells.
The listed abstract below showed that Tim-1 is more highly expressed on naive B cells than on T cells.
Depleting B cells led to Tim-1 accelerated islet cell rejection in these mice. Re constitution of B cells led to prolonged graft survival and and transfer of Tim-1 + B cells prolonged allograft survivial suggesting that Tim-1 + b cells could be B regulatory cells like Foxp3+ T reg cells.
Again, no human data yet. more studies to come!
Exciting stuff!
Reference:
Ding Q, Yueng M, Najafian N, et al. Regulatory B cells are identified by TIM-1 and can be induced through TIM-1 ligation to promote allograft survival. ATC 2010, San Diego, Calif, Abstract 167.
Infections post transplant
We had a good discussion about infections post transplant yesterday ranging from rare cases of Parvovirus B19 to common bacterial infections
A timeline is important to keep in mind.
<1Month into transplant
Think of the common post surgical fever causes
MRSA, Pneumonias
Wound infection
C.diff
Aspiration
BKV can be seen as early as 2 weeks( depending on net immunosuppression state of the patient)
1-6 months into transplant
BK Nephritis
Adenovirus
CMV, PCP
HCV
MAC
>6 months
Back to normal population infections
But also
Nocardia
Atypical fungi
West nile
JC virus( PML)
CMV can happen here as well
So can BKV
A nice review is listed below from NEJM
http://www.ncbi.nlm.nih.gov/pubmed/18094380
A timeline is important to keep in mind.
<1Month into transplant
Think of the common post surgical fever causes
MRSA, Pneumonias
Wound infection
C.diff
Aspiration
BKV can be seen as early as 2 weeks( depending on net immunosuppression state of the patient)
1-6 months into transplant
BK Nephritis
Adenovirus
CMV, PCP
HCV
MAC
>6 months
Back to normal population infections
But also
Nocardia
Atypical fungi
West nile
JC virus( PML)
CMV can happen here as well
So can BKV
A nice review is listed below from NEJM
http://www.ncbi.nlm.nih.gov/pubmed/18094380
Labels:
Infections,
post transplant complications
Wednesday, September 22, 2010
Quiz 6 answers
Which is true? 1.The incidence of Kaposi Sarcoma is most highest in liver transplants of all solid organ transplants | |||
2.Females are more of risk than males get Kaposi Sarcoma in Renal transplant patients | |||
3.It is caused by Human Herpes virus 6 4.Most cases of Kaposi's Sarcoma occur in individuals of Mediterranean or Arabic origin
| |||
Labels:
post transplant complications,
quiz
Tuesday, September 21, 2010
Renal Fellow Network: Doc, I am very sensitized! (part 2)
Renal Fellow Network: Doc, I am very sensitized! (part 2): "Let’s continue our discussion from our last blog about sensitized kidney recipients. In summary, we have this 60 yo man interested on a seco..."
Renal Fellow Network: Doc, I am very sensitized!
Renal Fellow Network: Doc, I am very sensitized!: "Another day of transplant clinic… I heard from my attending that a couple is here for a second opinion about a kidney transplant. The husban..."
Friday, September 17, 2010
Sunday, September 12, 2010
Can BK Virus serum PCR be a good marker for Net immunosuppression?

In the field of transplantation, we are struggling to figure out is the patient on which end of the spectrum, too little immunosuppresion or too much immunosuppression. Markers for rejection have been studied extensively and based on Luminex DSA one can monitor early signs of impending antibody rejection. But many centers are also developing aggressive screening strategies for BK Nephritis. This entity is usually seen as early as 2 weeks post transplant to as late as 7 years post transplant but usually in the first year or so.
I think that A BK serum PCR might be a good marker for NET immunosuppression. Someone who has lupus and has been treated with Cytoxan, Cellcept, Rituxan and has failed kidneys recently and then gets a transplant for the kidney and gets inducted with more immunosuppression might be the highest risk for BK Nephritis much earlier on due to their NET immunosuppresion being the highest. No one can really measure NET immunsuppression. There is a test available called " Cylex" or ImmuKnow . This is the physiology behind it:
"Phytohemagglutinin (PHA) is a non‐specific mitogen which can be used to stimulate cell division in CD4 T‐ lymphocytes regardless of their antigenic specificity or memory status. Therefore, PHA is considered to be a “global” stimulator of the immune system. The production of intracellular ATP is one of the first steps in cellular activation following stimulation with mitogens such as PHA. ATP is a multifunctional nucleotide which plays an indispensible role in the transfer of intracellular chemical energy. The amount of ATP generated can tell us the amount of CD4 T cell activation and the overall immune status of the patient( over or under immunosuppressed). " -from the cylex website( summarized)
But a cell activation can occur in setting on an infection as well and a similar down stream effect on the kidney. Steady monitoring of infectious agents like BKV might be the BEST marker we have to date to tell us " Hey there is too much immunosuppression on board" !
But might not be as simple as that...
Lets see what future studies hold...
Cidofivir for BK Nephritis
 As we all know that treatment for BK Nephritis is tough. The only thing that really works well is Decreasing immunosuppresion. But as we do that, the risk of mounting an immune response arises and you can start seeing biopsies that look like Acute Cellular Rejection and BK staining Positive.
As we all know that treatment for BK Nephritis is tough. The only thing that really works well is Decreasing immunosuppresion. But as we do that, the risk of mounting an immune response arises and you can start seeing biopsies that look like Acute Cellular Rejection and BK staining Positive. At that time, most people will treat with IV Immunoglobulins and see if there is some response in terms of preventing rejection and treating BK at the same time.
So far, no drug has directly targeted BK except Cidofivir. Cidofovir is an antiviral agent that demonstrates in vitro activity against murine polyomavirus and has been proposed for treatment of BKVN in renal allograft recipients. The dose usually recommended is 0.25mg/kg IV every 2 weeks for 8 doses total. This is a low dose and can be used for someone in already some graft dysfunction as cidofivir itself can causing ATN like injury( same as tenofivir). This low-dose cidofovir may be tolerated, even among renal transplant recipients with significant renal dysfunction due to BKVN. Prospective, controlled trials are warranted to further define the optimal dose, toxicity and potential role of cidofovir in renal transplant recipients with BK virus nephropathy.
http://www.ncbi.nlm.nih.gov/pubmed/18380832
http://www.ncbi.nlm.nih.gov/pubmed/16499584
Labels:
BK virus,
Infections,
post transplant complications
Thursday, September 9, 2010
Paired Chain Donation
A nice letter to the editor in NEJM this week Sept 2010 reflects on the Kidney Paired Donation program from San Antonio, Texas. KPD, which matches a living donor with a compatible recipient in a tag-team approach among potential donor–recipient pairs, can achieve compatible transplant combinations.
Based on this letter, if performed at a national level, it would potentially result in approximately 2000 additional live-donor transplantations annually and reduce the number of patients on the waiting list.
This is a growing trend and many transplant centers are reaching out to do this in many different ways. Some via a paired donation and some via a chain that is started by an altruistic donor.
Have a look at the NEJM editorial
http://www.nejm.org/doi/full/10.1056/NEJMc1004959
http://www.ncbi.nlm.nih.gov/pubmed/20061914
Based on this letter, if performed at a national level, it would potentially result in approximately 2000 additional live-donor transplantations annually and reduce the number of patients on the waiting list.
This is a growing trend and many transplant centers are reaching out to do this in many different ways. Some via a paired donation and some via a chain that is started by an altruistic donor.
Have a look at the NEJM editorial
http://www.nejm.org/doi/full/10.1056/NEJMc1004959
http://www.ncbi.nlm.nih.gov/pubmed/20061914
Labels:
clinical science,
kidney transplantation
Tuesday, September 7, 2010
Quiz 5 Answers
Which one of the following is not a risk factor for PTLD
EBV status of donor/recipient 2 (16%)
Prior malignancy 1 (8%)
"Net" immunosuppresion 1 (8%)
Prior BK Virus infection 6 (50%)
Age 2 (16%)
Most of you got this one right away!
All except Prior BK infection has been associated to be a risk factor for PTLD In kidney transplant recipients
Please review the recent updated PTLD presentation by Arun Chawla for further clarification
http://onlinetransplantcenter.blogspot.com/search/label/presentations
EBV status of donor/recipient 2 (16%)
Prior malignancy 1 (8%)
"Net" immunosuppresion 1 (8%)
Prior BK Virus infection 6 (50%)
Age 2 (16%)
Most of you got this one right away!
All except Prior BK infection has been associated to be a risk factor for PTLD In kidney transplant recipients
Please review the recent updated PTLD presentation by Arun Chawla for further clarification
http://onlinetransplantcenter.blogspot.com/search/label/presentations
Labels:
cancer,
post transplant complications,
quiz
Monday, September 6, 2010
Post Kidney Transplant Renal Injury!
A Short Reminder!
We encounter acute renal failure always in the post transplant period
Besides the traditional pre renal, renal and post renal way of looking at the causes of renal injury post transplant, a mnemonic I learned from my mentors was : SCRI
or short for serum creatinine.
S- STRUCTURAL CAUSES
C- Calcineurin Toxicity
R- Rejection, any type/ Recurrence of primary disease
I- Infection, usually BK
The causes of proteinuria post transplant( major causes)
Rejection
Recurrence
De novo Glomerular Disease
Transplant Glomerulopathy
Post Transplant Collapsing FSGS
We encounter acute renal failure always in the post transplant period
Besides the traditional pre renal, renal and post renal way of looking at the causes of renal injury post transplant, a mnemonic I learned from my mentors was : SCRI
or short for serum creatinine.
S- STRUCTURAL CAUSES
C- Calcineurin Toxicity
R- Rejection, any type/ Recurrence of primary disease
I- Infection, usually BK
The causes of proteinuria post transplant( major causes)
Rejection
Recurrence
De novo Glomerular Disease
Transplant Glomerulopathy
Post Transplant Collapsing FSGS
Friday, August 27, 2010
CMV infection in Kidney Transplantation
Here is a brief presentation by Arun Chawla, MD on CMV in Kidney Transplantation.
CMV in Organ Transplantation
View more presentations from Nephrology, NSLIJ.
Thursday, August 26, 2010
Interferon Gamma use in fungal infections in transplant patients
A recent article in AJT reports the use of Interferon Gamma as a salvage and additional therapy for disseminated fungal infections in kidney transplant recipients.
We always get concerned with giving interferons to transplant recipients as it will increase and promote an immune response and pose a risk of rejection.
In the above cases, not only did the patients survived but the graft was not effect in 4/7 cases as well with no consequences of rejection. Why interferon gamma? It is the most important cytokine in communication of T cells to fight fungal and mycobacterial infections.
The idea is novel yet scary. More data and more cases are needed till we think of possibly using this in large clinical settings. Clearly, the concern of activating more crosstalk among T helper cells by using Interferon Gamma is helpful in fighting infection but might have to be the right balance to prevent rejection.
Reference:
http://www.ncbi.nlm.nih.gov/pubmed/20353472
http://www.ncbi.nlm.nih.gov/pubmed/20636453
We always get concerned with giving interferons to transplant recipients as it will increase and promote an immune response and pose a risk of rejection.
In the above cases, not only did the patients survived but the graft was not effect in 4/7 cases as well with no consequences of rejection. Why interferon gamma? It is the most important cytokine in communication of T cells to fight fungal and mycobacterial infections.
The idea is novel yet scary. More data and more cases are needed till we think of possibly using this in large clinical settings. Clearly, the concern of activating more crosstalk among T helper cells by using Interferon Gamma is helpful in fighting infection but might have to be the right balance to prevent rejection.
Reference:
http://www.ncbi.nlm.nih.gov/pubmed/20353472
http://www.ncbi.nlm.nih.gov/pubmed/20636453
Wednesday, August 25, 2010
Quiz 4 Answers
What is the most common cause of Denovo Thrombotic Microangiopathy post renal transplant?
Calcineurin inhibitor toxicity 5 (55%)
Antibody mediated rejection 3 (33%)
MPGN 0 (0%)
Malignancy 0 (0%)
Infections 1 (11%)
Denovo TMA post transplant is defined as happening in the early post transplant period.( 6 months). All of the above can cause de novo TMA in post transplant patients. The most common cause as most of you got it is CNI toxicity. Although, Antibody mediated rejection closely follows it and should always be considered. Another cause not listed here is ischemic repefusion injury as well leading to a TMA.
A recent study in AJT August 2010 showed in a retrospective fashion that TMA can be very strongly associated with C4D positive Biopsies showing ABMR as well. 14% with CD4 positive patients had TMA compared to only 3% with C4D negative biopsies. Treatment changes - Plasmapheresis might help in this case as you will remove the donor specific antibodies and also help the process of TMA treatment.
Regardless in any case of TMA, treat the underlying cause if found! CNI induced TMA doesn't NEED to be treated with plasmapheresis
References:
http://www.ncbi.nlm.nih.gov/pubmed/20659088
Calcineurin inhibitor toxicity 5 (55%)
Antibody mediated rejection 3 (33%)
MPGN 0 (0%)
Malignancy 0 (0%)
Infections 1 (11%)
Denovo TMA post transplant is defined as happening in the early post transplant period.( 6 months). All of the above can cause de novo TMA in post transplant patients. The most common cause as most of you got it is CNI toxicity. Although, Antibody mediated rejection closely follows it and should always be considered. Another cause not listed here is ischemic repefusion injury as well leading to a TMA.
A recent study in AJT August 2010 showed in a retrospective fashion that TMA can be very strongly associated with C4D positive Biopsies showing ABMR as well. 14% with CD4 positive patients had TMA compared to only 3% with C4D negative biopsies. Treatment changes - Plasmapheresis might help in this case as you will remove the donor specific antibodies and also help the process of TMA treatment.
Regardless in any case of TMA, treat the underlying cause if found! CNI induced TMA doesn't NEED to be treated with plasmapheresis
References:
http://www.ncbi.nlm.nih.gov/pubmed/20659088
Friday, August 20, 2010
B cell and long term graft function
A lot of transplant patients do so well and require very minimal amounts of medications. What is the magic recipe for that? Perhaps it is T regs cells and amount of T regs vs T effector cells. Perhaps it is a subset of B cells.
A recent paper in Kidney International addresses this topic.
The investigators compared B cells of people with stable graft function and ones with chronic rejection and healthy volunteers. They found that the ones who had stable graft function with minimal drugs had increased B cells of activated, memory and early memory type. They had a enriched transcriptional profiling. The costimulatory molecules like CD40 and CD80 ligand were upregulated in these B cells. These cells were also giving out an inhibitory signal for proliferation and a preventive signal for Hyperactive B cell response. They expressed CD1D and CD5 ( another recent paper had suggested this as well).
This suggests that there a specific type of B cells out there that patients with good graft function and minimal drugs have that might be regulatory in nature and allow long term graft functioning.
More studies should be done to look out for these type of cells
http://www.ncbi.nlm.nih.gov/pubmed/20531452
Also, perhaps using anti co stiumatory blockades might not be all that ideal then? Perhaps. not much data to say yes or no!
A recent paper in Kidney International addresses this topic.
The investigators compared B cells of people with stable graft function and ones with chronic rejection and healthy volunteers. They found that the ones who had stable graft function with minimal drugs had increased B cells of activated, memory and early memory type. They had a enriched transcriptional profiling. The costimulatory molecules like CD40 and CD80 ligand were upregulated in these B cells. These cells were also giving out an inhibitory signal for proliferation and a preventive signal for Hyperactive B cell response. They expressed CD1D and CD5 ( another recent paper had suggested this as well).
This suggests that there a specific type of B cells out there that patients with good graft function and minimal drugs have that might be regulatory in nature and allow long term graft functioning.
More studies should be done to look out for these type of cells
http://www.ncbi.nlm.nih.gov/pubmed/20531452
Also, perhaps using anti co stiumatory blockades might not be all that ideal then? Perhaps. not much data to say yes or no!
Labels:
Basic Science,
clinical science,
Immunology
Monday, August 16, 2010
Transplantatation of two kidneys in marginal donors
http://nephrohug.com/2010/08/16/greffe-des-deux-reins/
Check out the above French Blog on this topic from Nephrohug.
Check out the above French Blog on this topic from Nephrohug.
Labels:
clinical science,
donors,
kidney transplantation
Friday, August 13, 2010
The Micro RNA blog
Take a look at this extensive summaries of blogs just on micro RNAs
Very neat blog
http://mirnablog.com/
Very neat blog
http://mirnablog.com/
Labels:
Basic Science,
Education,
Immunology
Wednesday, August 11, 2010
BKV viral protein-1 mRNA in urinary cells
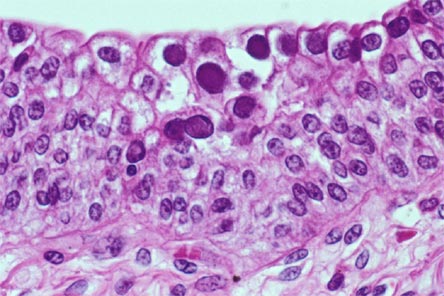
A noninvasive, accurate biomarker for diagnosis of BKVN is being sought. Recent article in Transplantation reports using the urinary cell mRNA profile at the time of BK Nephropathy diagnosis and compared to risk of graft function.
BK Nephropathy was diagnosed with a sensitivity of 100% and specificity of 97% using the urinary mRNA. Levels of granzyme B (GB) mRNA and proteinase inhibitor (PI)-9 mRNA in urinary cells were higher in BKV patients with a subsequent decline in renal function compared with patients with stable function, and were positively associated with rise in serum creatinine from the time of BK diagnosis to 12 months after diagnosis.
This confirms the fact that urinary granzyme B and PI-9 could be used as markers of inflammation during any renal episode post transplant. Similar findings were seen in rejection as well. It seems that no matter what causes the inflammation, BK or rejection, a rise in urinary GB and PI-9 suggests a poor prognosis.
Reference:
Wednesday, August 4, 2010
Low Donor Kidney Weight ? Does it matter?
We have asked this question many times in conferences and especially when a pediatric kidney gets put in an adult recipient? Does it matter if the donor kidney weight is not compatible to the recipient's weight?
There is one study in 2005 that showed that low donor kidney weight to recipient weight ratio did not affect graft survival. That study only had 2.5 year follow up.
A recent study in JASN looked at >1000 patients for over 10 years and max of 7 year follow up. They found that with a low donor kidney to recipient kidney ratio of <2.3g/kg, initially the GFR increased, plateaued at 6 months but then decreased rapidly after 7 years at a mean rate of 3 ml/min.
With patients with >2.3g/kg, the the GFR after 7 years decreased at a much slower rate- 1.34ml/min.
The proteinuria was also higher in the low ratio group.FSGS was more common in the biopsies of the low ratio group.This is a retrospective analysis with its usual flaws but raises an important point of avoiding kidney and recipient weight incompatibility to avoid late clinical outcomes.
References:
http://www.ncbi.nlm.nih.gov/pubmed/20488949
http://www.ncbi.nlm.nih.gov/pubmed/15563571
There is one study in 2005 that showed that low donor kidney weight to recipient weight ratio did not affect graft survival. That study only had 2.5 year follow up.
A recent study in JASN looked at >1000 patients for over 10 years and max of 7 year follow up. They found that with a low donor kidney to recipient kidney ratio of <2.3g/kg, initially the GFR increased, plateaued at 6 months but then decreased rapidly after 7 years at a mean rate of 3 ml/min.
With patients with >2.3g/kg, the the GFR after 7 years decreased at a much slower rate- 1.34ml/min.
The proteinuria was also higher in the low ratio group.FSGS was more common in the biopsies of the low ratio group.This is a retrospective analysis with its usual flaws but raises an important point of avoiding kidney and recipient weight incompatibility to avoid late clinical outcomes.
References:
http://www.ncbi.nlm.nih.gov/pubmed/20488949
http://www.ncbi.nlm.nih.gov/pubmed/15563571
Labels:
clinical science,
donors,
kidney transplantation
Tuesday, August 3, 2010
Post transplant TMA, revisiting Atypical HUS
Post Transplantation is a real entity. Many causes have been identified. CNI toxicity, Sirolimus, ischemia, antibody mediated rejection or de novo carcinoma, antiphospholipid syndrome, post transplant SLE are a few possible diagnosis. One study showed that among 24 patients with post transplant TMA that was de novo, 7 carried a mutation in CFH or CFI or combined mutation, indicating a genetic abnormality that might be the first hit.
In the past decade, work has been very active in the field of Atypical HUS. Many complement abnormalities have been identified namely the CFH , CFI mutations, C3 mutations, CFB mutations, all which are mutations in the alternative pathway of complement leading to activation of MAC and TMA
A recent review in AJT July 2010 issue makes the following recs:
1. Screening for the above mutations to be done with all patients with aHUS prior to transplatation. I think that perhaps any non diarrheal related HUS should be screened as this might be the first hit.
2. Avoid Living related donation in such positive cases due to genetic transmission. Suggest a friend or spouse in such cases.
3. Studies have shown that aHUS MCP mutation can undergo kidney transplantation without increase risk of recurrence.
4. Anti CFH mutations might need pre emptive plasmapheresis, rituximab and steroids to lower the antibody levels.
5. The CFH and CFI mutations, the risk of recurrence is very high and transplant might be a risky procedure.
6. The options for CFH and CFI mutations might be combined liver-kidney transplantion along with TPE pre and post. Kidney alone with Pre and post TPE or kidney alone with eculizumab( anti complement agent).
All are only cases described, so no final decisions can be made. risk benefit has to be discussed with each case. Similar situations play part in C3 and CFB mutations as well. THBD mutations also are at risk but there is no data to do anything in these cases.
Does Nephrectomy of native kidneys help? Again, doesn't seem to be beneficial.
Check out these references:
http://www.ncbi.nlm.nih.gov/pubmed/20642678
http://www.ncbi.nlm.nih.gov/pubmed/20445192
http://www.ncbi.nlm.nih.gov/pubmed/20595690
Image source: http://www.profelis.org/amc/vorlesungen/immunologie/komplementsystem.html
Monday, July 26, 2010
Hematuria and Donation?
Donating a kidney is a very noble thought. We usually screen for hematuria in the donors. Aysmptomatic hematuria is 13% in general population. Are donors with asymptomatic hematuria safe to donate?
This question is a tough one with no specific answers. A recent study in AJT July 2010 tries to answer this question in a retrospective study. 8.3% of kidney donors in 8 years of their evaluation had persistent hematuria pre donation that increased to 15% after donation and when persistent was associated with hypertension, proteinuria and renal damage. The authors go ahead and conclude that donation of someone with persistent hematuria is not ideal. What is persistent? Months or Years? Its usually on repeated testing at this point. Can be more than 2-3 tests in a short period of time or long period of time.
An editorial in the same issue takes a look at this question of possible donation in such cases.
An approach is suggested( no evidence but just opinion)
1. Repeat testing , assess for proteinuria and a 24 hour CRCL to make sure there is no renal damage. any indication of the above two would halt the donation
2. Nephrology assessment independent of the transplant center as a donor advocate.
3. Role of kidney biopsy might be helpful to help discern an occult IgA Nephropathy or genetic diseases such as Alport's Disease. Family members who have hematuria who are donating should raise concerns of potential genetic causes that might be the same cause in the recipient.
Living donor Transplants from relatives in Alport families is an ambivalent option. Based on one study in NDT 2009, proteinuria should be an exclusion criterion. Even in these donors with isolated hematuria, families and their physicians should be aware of an increased risk of renal failure in donor and recipient. Careful donor evaluation with a potential need of kidney biopsy might help make the decision easier.
This is a tough question that is hard to answer with any hard data. If there is alternate donor with NO hematuria, that would be ideal.
Ref:
http://www.ncbi.nlm.nih.gov/pubmed/20353466
http://www.ncbi.nlm.nih.gov/pubmed/20642672
http://www.ncbi.nlm.nih.gov/pubmed/19028755
This question is a tough one with no specific answers. A recent study in AJT July 2010 tries to answer this question in a retrospective study. 8.3% of kidney donors in 8 years of their evaluation had persistent hematuria pre donation that increased to 15% after donation and when persistent was associated with hypertension, proteinuria and renal damage. The authors go ahead and conclude that donation of someone with persistent hematuria is not ideal. What is persistent? Months or Years? Its usually on repeated testing at this point. Can be more than 2-3 tests in a short period of time or long period of time.
An editorial in the same issue takes a look at this question of possible donation in such cases.
An approach is suggested( no evidence but just opinion)
1. Repeat testing , assess for proteinuria and a 24 hour CRCL to make sure there is no renal damage. any indication of the above two would halt the donation
2. Nephrology assessment independent of the transplant center as a donor advocate.
3. Role of kidney biopsy might be helpful to help discern an occult IgA Nephropathy or genetic diseases such as Alport's Disease. Family members who have hematuria who are donating should raise concerns of potential genetic causes that might be the same cause in the recipient.
Living donor Transplants from relatives in Alport families is an ambivalent option. Based on one study in NDT 2009, proteinuria should be an exclusion criterion. Even in these donors with isolated hematuria, families and their physicians should be aware of an increased risk of renal failure in donor and recipient. Careful donor evaluation with a potential need of kidney biopsy might help make the decision easier.
This is a tough question that is hard to answer with any hard data. If there is alternate donor with NO hematuria, that would be ideal.
Ref:
http://www.ncbi.nlm.nih.gov/pubmed/20353466
http://www.ncbi.nlm.nih.gov/pubmed/20642672
http://www.ncbi.nlm.nih.gov/pubmed/19028755
Labels:
clinical science,
donors,
kidney transplantation
Friday, July 23, 2010
Wednesday, July 21, 2010
Micro RNAs and Transplantation
A novel concept has been emerging in the last few years regarding micro RNAs. It already has reached some human data in transplant patients.
What is micro RNA? These are non coding areas of the RNA that play a critical role in regulation of gene expression. They might alter the structure and lead to either expression or regression of the protein in question.
There is mice data that microRNAs play a role in immune response, adaptive immunity, inflammation, fibrosis and epithelial changes. The role of microRNA will help us understand intracellular signalling, expression of proteins, modulation of cytokines, and graft response better.
Few simple examples are: miR 155 regulates immune response to bacterial infections and viral infections and helps in the crosstalk macrophage becoming an activated macrophage. Myeloid stem cell goes to becoming a mast cell due to miR 223; and so forth.
What is more fascinating is the role of this in Transplantation. How can this be useful in transplantation? they can be measured in serum, urine and plasma. Two studies have now shown that the micro RNA pattern in the in renal allograft biopsies is different in acute rejection episodes vs controls.
The future looks good:- These might be good panel of markers for allograft status. Therapeutic use of this application in altering the microRNA enviornment might be of advantage to prevent fibrosis or rejection.
Image source:
http://universe-review.ca/I11-38-microRNA.jpg
Good references:
http://www.ncbi.nlm.nih.gov/pubmed/20574417
http://www.ncbi.nlm.nih.gov/pubmed/18346642
http://www.ncbi.nlm.nih.gov/pubmed/19289845
What is micro RNA? These are non coding areas of the RNA that play a critical role in regulation of gene expression. They might alter the structure and lead to either expression or regression of the protein in question.
There is mice data that microRNAs play a role in immune response, adaptive immunity, inflammation, fibrosis and epithelial changes. The role of microRNA will help us understand intracellular signalling, expression of proteins, modulation of cytokines, and graft response better.
Few simple examples are: miR 155 regulates immune response to bacterial infections and viral infections and helps in the crosstalk macrophage becoming an activated macrophage. Myeloid stem cell goes to becoming a mast cell due to miR 223; and so forth.
What is more fascinating is the role of this in Transplantation. How can this be useful in transplantation? they can be measured in serum, urine and plasma. Two studies have now shown that the micro RNA pattern in the in renal allograft biopsies is different in acute rejection episodes vs controls.
The future looks good:- These might be good panel of markers for allograft status. Therapeutic use of this application in altering the microRNA enviornment might be of advantage to prevent fibrosis or rejection.
Image source:
http://universe-review.ca/I11-38-microRNA.jpg
Good references:
http://www.ncbi.nlm.nih.gov/pubmed/20574417
http://www.ncbi.nlm.nih.gov/pubmed/18346642
http://www.ncbi.nlm.nih.gov/pubmed/19289845
Labels:
Basic Science,
Immunology,
kidney transplantation
Friday, July 16, 2010
Transplant/Immunology Quiz 3 answers
HLA Mismatch 20%
CMV infection 40%
Hep C infection 40%
Sirolimus 40%
Calcium Channel Blockers 10%
Hypomagnesemia 20%
Elevated uric acid 30%
CNI use 70%
Metabolic syndrome 70%
NODAT is a common metabolic complication seen in post transplant patients as we are seeing these patients living longer and longer.
It has been linked independently as a risk factor for cardiac disease post transplant.
Lot of research has been done in this field and numerous physicians have done work on identifiable risk factors and hoping to decrease its
incidence.
The list I am going to put below is from a recent review in Nature Review Nephrology and might not be wholesome but covers most of the
known risk factors.
The non modifiable ones are: Age, African american race, Family history of DM, DM as a cause of ESRD. Interestingly, patients with
Glomerulonephritis and ADPKD leading to ESRD had increased risk of NODAT, male gender, HLA mismatch( weak association),
genetic, innate immunity( alteration in it post transplant), cadaveric donor, male donor, education.
The modifiable risk factors are: Previous stress related diabetes, obesity, metabolic syndrome, post transplant high TG level, CMV infection
(affecting the Beta cells directly), Hep C infection, tacrolimus > cyclosporine( direct pancreas effect), sirolimus, steroids, rejection episodes( perhaps
due to more steroid use), anti hypertensives( beta blockers, HCTZ), hypomagnesemia( 2 studies so far), hyperurecemia( one study so far), decreased
GFR.
This is interesting to me personally and we have showed ( in a very small study) that hypomagnesemia might be related to RAPID NODAT, within the
first three months of transplant. There is one large study out of Europe that showed this link before and there is animal and human data on direct
association of insulin resistance and hypomagnesemia as well.
Some good references:
http://www.ncbi.nlm.nih.gov/pubmed/20498675
http://www.ncbi.nlm.nih.gov/pubmed/17198258
http://www.ncbi.nlm.nih.gov/pubmed/20177345
http://www.ncbi.nlm.nih.gov/pubmed/15023151
http://www.ncbi.nlm.nih.gov/pubmed/19624560
http://www.renalandurologynews.com/new-onset-diabetes-linked-to-post-transplant-hypomagnesemia/article/169297/
Wednesday, July 14, 2010
Leflunomide and liver failure
The FDA just expanded the black box warning on leflunomide( ARAVA), a drug that is sometimes used to treat BK Nephritis in Transplant patients. A recent report showed 49 cases of severe liver toxicity from 2002-2009. Usually the reactions were noted in the first 12 months post use of the drug. The greatest risk occurred in patients taking other drugs that may cause liver damage while taking leflunomide and in patients with preexisting liver disease.
This comes as a shock to some of us in the transplant community as we do use this medication for treatment of BK Nephritis. There is so little in the form of treatment available for BK, this black box warning might make leflunomide not a very user friendly drug anymore.
Sunday, July 11, 2010
Lupus Nephritis Post Transplant
We have asked this questions many times? Every center gives different answers. Some people have different experiences about this topic. When a lupus nephritis associated ESRD patient gets a kidney transplant, what is the risk of recurrence of lupus in the transplanted kidney?
Well, the recent issue of JASN highlights this question. From the UNOS database, 6850 patients who had lupus induced kidney diseases and then a transplant was done were reviewed. Only 167 of them had recurrent lupus. The amount is very small. Three risk factors were identified:
1. African American Recipients.
2. Female recipient.
3. Younger recipient.
As we all think, most of the low numbers of recurrence is likely because we use the same medications that we use for transplant, also to treat and keep lupus under control.
Take a peek at this paper.
http://www.ncbi.nlm.nih.gov/pubmed/20488956
Well, the recent issue of JASN highlights this question. From the UNOS database, 6850 patients who had lupus induced kidney diseases and then a transplant was done were reviewed. Only 167 of them had recurrent lupus. The amount is very small. Three risk factors were identified:
1. African American Recipients.
2. Female recipient.
3. Younger recipient.
As we all think, most of the low numbers of recurrence is likely because we use the same medications that we use for transplant, also to treat and keep lupus under control.
Take a peek at this paper.
http://www.ncbi.nlm.nih.gov/pubmed/20488956
Tuesday, July 6, 2010
Organ Trading Discussion
The Economist is holding a live debate on Organ trading on Facebook.
Check it out with this link On facebook.
Also, the Renal Fellow Network has a recent post on it as well.
Check it out with this link On facebook.
Also, the Renal Fellow Network has a recent post on it as well.
Labels:
clinical science,
donors,
Education
Monday, July 5, 2010
Photopheresis therapy for renal allograft rejection?
The technique involves three stages: 1-leucapheresis, 2- photoactivation with photosensitizer plus UV A irradiation, and 3- re-infusion of the buffy coat.
Extra Corporal Photopheresis (ECP) was first introduced for the treatment of Cutaneous T-Cell Lymphoma. Now has been widely used in the treatment of acute allograft rejection; most extensively in cases of cardiac transplant rejection. It has also shown success and high efficacy in reversing renal allograft rejection as well. Only one cohort study has been done by Jardine et al; ECP been used in 10 kidney recipients with therapy resistant rejection, and to our surprise, it showed that rejection has been resolved in all patients treated with ECP!
The exact mechanism of action remains unclear, but believe it has an immunomodulatory rather than immunosuppressive effect: The irradiation therapy induces high rate of apoptosis of the T-cells with sparing of the monocytes, and this eventually creates changes in the patient’s cytokine profile towards “type 2” cytokines; with significant increase of IL-5 and decrease of IFN-Gamma - “which is associated with allograft rejection!” also, it has a stimulatory effect on the T-regulatory cells as well..
Safety profile is excellent with <1% adverse effect, considered more safe than any other modality of apheresis!
ECP been mainly used for CTCL, and GVHD. Also, has been used in other autoimmune diseases including MS, scleroderma, DM-1, RA, psoriasis, Crohn’s, Nephrogenic Fibrosing Dermopathy. ECP is an effective, tolerable, and safe immunomodulatory therapy that can be used theoretically for resistant renal allograft rejection “T-cell rejection”. We still need more data and large cohort trials for this promising technique/therapy.
Extra Corporal Photopheresis (ECP) was first introduced for the treatment of Cutaneous T-Cell Lymphoma. Now has been widely used in the treatment of acute allograft rejection; most extensively in cases of cardiac transplant rejection. It has also shown success and high efficacy in reversing renal allograft rejection as well. Only one cohort study has been done by Jardine et al; ECP been used in 10 kidney recipients with therapy resistant rejection, and to our surprise, it showed that rejection has been resolved in all patients treated with ECP!
The exact mechanism of action remains unclear, but believe it has an immunomodulatory rather than immunosuppressive effect: The irradiation therapy induces high rate of apoptosis of the T-cells with sparing of the monocytes, and this eventually creates changes in the patient’s cytokine profile towards “type 2” cytokines; with significant increase of IL-5 and decrease of IFN-Gamma - “which is associated with allograft rejection!” also, it has a stimulatory effect on the T-regulatory cells as well..
Safety profile is excellent with <1% adverse effect, considered more safe than any other modality of apheresis!
ECP been mainly used for CTCL, and GVHD. Also, has been used in other autoimmune diseases including MS, scleroderma, DM-1, RA, psoriasis, Crohn’s, Nephrogenic Fibrosing Dermopathy. ECP is an effective, tolerable, and safe immunomodulatory therapy that can be used theoretically for resistant renal allograft rejection “T-cell rejection”. We still need more data and large cohort trials for this promising technique/therapy.
Friday, July 2, 2010
Live Donor Nephrectomy with vaginal extraction
Donor nephrectomies are being done in some patients via a different approach at John Hopkins. A case report was done for a patient presented in AJT July 2010 issue where the donor kidney was removed via vaginal route. The warm ischemia time was 3 min and the post op pain was less; hospital stay was shorter and the cosmetic outcome was more desirable. This is a creative approach to a surgical technique.
Lets see where we stand with this in the future.
For now its just one patient and we have to wait and see further work in this field. An editorial along with this case report is a must read as well. It discusses the potential hazards of this type of approach.
http://www.ncbi.nlm.nih.gov/pubmed/20553450
http://www.ncbi.nlm.nih.gov/pubmed/20353482
Lets see where we stand with this in the future.
For now its just one patient and we have to wait and see further work in this field. An editorial along with this case report is a must read as well. It discusses the potential hazards of this type of approach.
http://www.ncbi.nlm.nih.gov/pubmed/20553450
http://www.ncbi.nlm.nih.gov/pubmed/20353482
Labels:
clinical science,
donors,
kidney transplantation,
surgery
Thursday, July 1, 2010
Saturday, June 19, 2010
Answer to Immunology Quiz 2
Immunology Quiz 2:
Which of the following drug & target of action combinations incorrectly matched?
Responses:
Tacrolimus/Calcineurin - 16%
Basiliximab/CD3 - 66%
MMF/IMPDH - 8%
Sirolimus/mTOR - 16%
Belatacept/CD80,86 - 33%
Compath/CD52 - 8%
OKT3/CD25 - 66%
Answer:
As majority of you indicated, the incorrect combinations are Basiliximab/CD3 and OKT3/CD25. Basiliximab acts by blocking IL2 receptor, also known as CD25. OKT3 or Muromonab-CD3 is a monoclonal antibody to CD3 on T cells. 33% of you marked Belatacept/CD80,86 as incorrect combination. However, this is a wrong choice as CD80/86 on antigen presenting cells is indeed the target of action for Belatacept there by inhibiting CD28 costimulation pathway of T cell activation.
Which of the following drug & target of action combinations incorrectly matched?
Responses:
Tacrolimus/Calcineurin - 16%
Basiliximab/CD3 - 66%
MMF/IMPDH - 8%
Sirolimus/mTOR - 16%
Belatacept/CD80,86 - 33%
Compath/CD52 - 8%
OKT3/CD25 - 66%
Answer:
As majority of you indicated, the incorrect combinations are Basiliximab/CD3 and OKT3/CD25. Basiliximab acts by blocking IL2 receptor, also known as CD25. OKT3 or Muromonab-CD3 is a monoclonal antibody to CD3 on T cells. 33% of you marked Belatacept/CD80,86 as incorrect combination. However, this is a wrong choice as CD80/86 on antigen presenting cells is indeed the target of action for Belatacept there by inhibiting CD28 costimulation pathway of T cell activation.
Labels:
Immunology,
kidney transplantation,
quiz
Rituximab for induction?
A trial from Sweden was published last year in Transplantation. It was a prospective, double blind, randomized, placebo-controlled multicenter study on the efficacy and safety of rituximab as induction therapy, together with tacrolimus, mycophenolate mofetil, and steroids in kidney transplants. The primary endpoint was defined as acute rejection, graft loss, or death during the first 6 months. They randomized 140 patients and found no difference in rejection episodes, infection episodes. There was a tendency toward fewer and milder rejections during the first 6 months in the rituximab group. A commentary of this also got published in recent May issue of Transplantation.
More trials need to be done with this agent before we think it can be used as an induction agent. Trails of using it as an induction in lupus also have been done in Europe with promising results.
Other areas where it is being used in highly sensitized individuals to desensitize. In cases of historical cross matches that are positive. Rituximab is becoming standard drug to give patients with antibody mediated rejection.
More trials need to be done with this agent before we think it can be used as an induction agent. Trails of using it as an induction in lupus also have been done in Europe with promising results.
Other areas where it is being used in highly sensitized individuals to desensitize. In cases of historical cross matches that are positive. Rituximab is becoming standard drug to give patients with antibody mediated rejection.
Subscribe to:
Comments (Atom)












